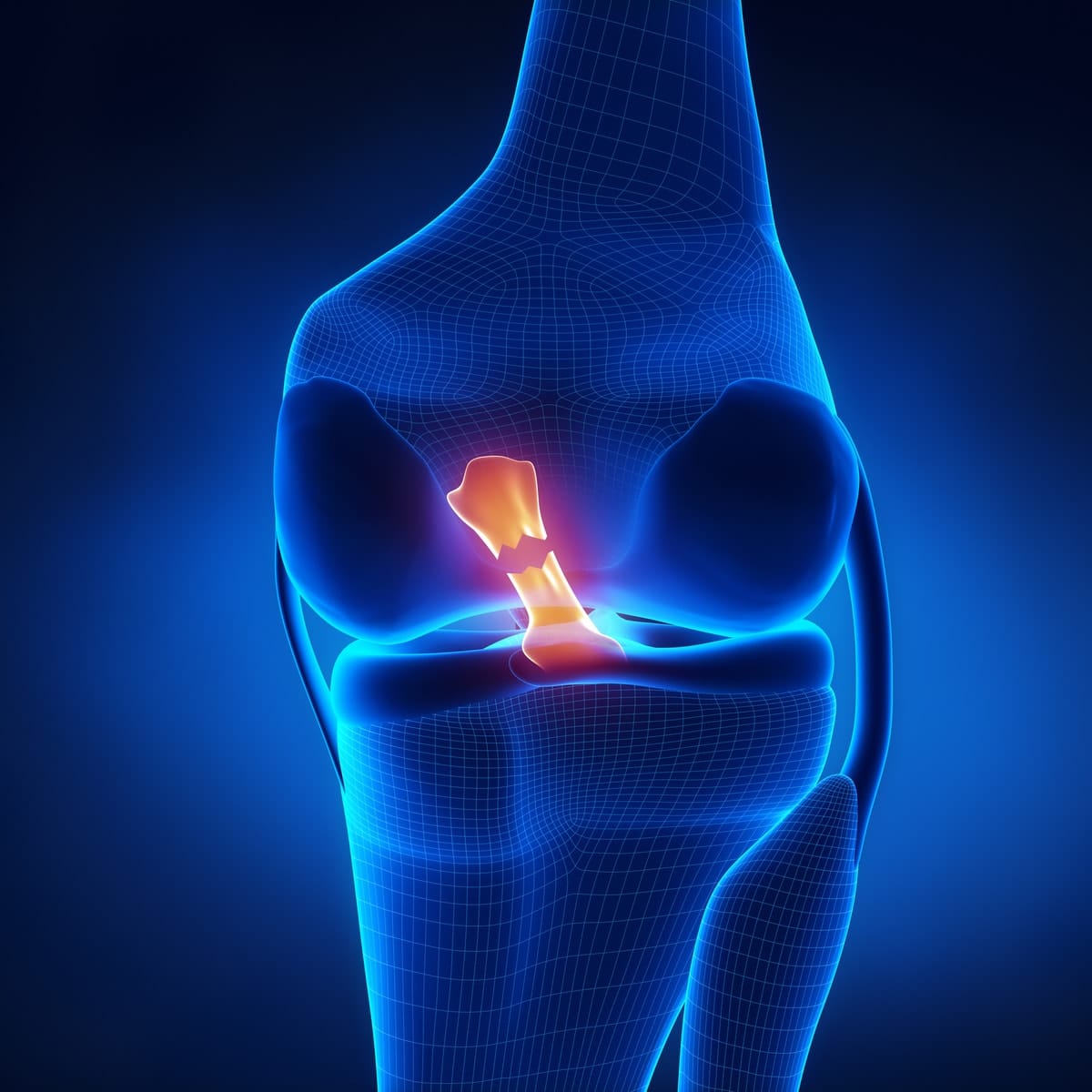
When Richmond key defender Alex Rance jumped to spoil a mark in the opening game of the 2019 Australian Football League season against Carlton, he landed as he had hundreds, probably thousands, of times before.
Only this time the consequence was different. When he landed, he clutched at his right knee, with confirmation later that he had ruptured his anterior cruciate ligament.
No one fell across him, he hadn’t landed awkwardly or hyper-extended his leg, and he had no history of knee injuries. He’d just … landed.
It was the first ACL injury of the 2019 AFL season, and it was barely an hour in. Since then, more than nine AFL footballers have injured their ACL, in addition to those such as Carlton co-captain Sam Docherty, who injured their knees in preseason matches or at training.
In the women’s league, the numbers are just as disturbing – Erin Phillips and Chloe Scheer in the same match, the 2019 AFLW Grand Final, No.1 draft pick Nina Morrison, Alex Williams and Brianna Moyes. All had their seasons cut short by ACL injuries.
But it isn’t just happening at the elite level. According to a study published last year in the Medical Journal of Australia, the number of young Australians requiring knee reconstructions in the previous 15 years rose 70 per cent. The greatest increase was in children under 14.
Almost 200,000 ACL reconstructions were performed during the study period, while the direct hospital costs of reconstructions for a single year, 2014-15, was estimated to be $142 million.
It’s a global trend, with more than two million injuries worldwide annually.
In the United States, there are approximately 200,000 ACL injuries every year, and, like Australia, it’s rising among young people and professional athletes, particularly in sports such as the NBA and NFL competitions.
Investigating fatigue
In the search for answers to what’s been described as a global sporting “epidemic”, a group of academics from the University of Michigan in 2013 began investigating whether material fatigue, or accumulated ACL microdamage at a molecular level, rather than a single-force incident, could be to blame for ACL failure during normal athletic activity.
They argue that just as bridges, aircraft and machine components can, over time and with repeated use, suffer from material fatigue and fail at stress levels considerably lower than their tensile or yield strength, so too might this be the case with many ACL injuries, given that 70 per cent of them are non-contact.
Their research has just been published in The American Journal of Sports Medicine.
Led by orthopaedic surgeon Edward Wojtys and biomechanical engineer James Ashton-Miller, both from the University of Michigan, the team tested one knee from each of seven adult cadavers in a controlled laboratory study using a purpose-built machine in which the knees were subjected to repetitive pivot landings loaded under four-times body weight – that’s about the weight under which someone jumps and lands.
What they found was that some of the ACLs began to fail under normal stress loads, but they didn’t know what the nature of the damage was that led to the failure.
Delving deeper
Professor Mark Banaszak Holl, who joined Monash University in January 2018 as head of chemical engineering, worked at the University of Michigan between 1995 and 2017, and was recruited onto the ACL project by Edward Wojtys to try and answer that question.
One of his research focuses is the structure and properties of biological materials, including ligaments. He’s continued to work with the Michigan team since arriving at Monash, and brought with him PhD student Jinhee Kim.
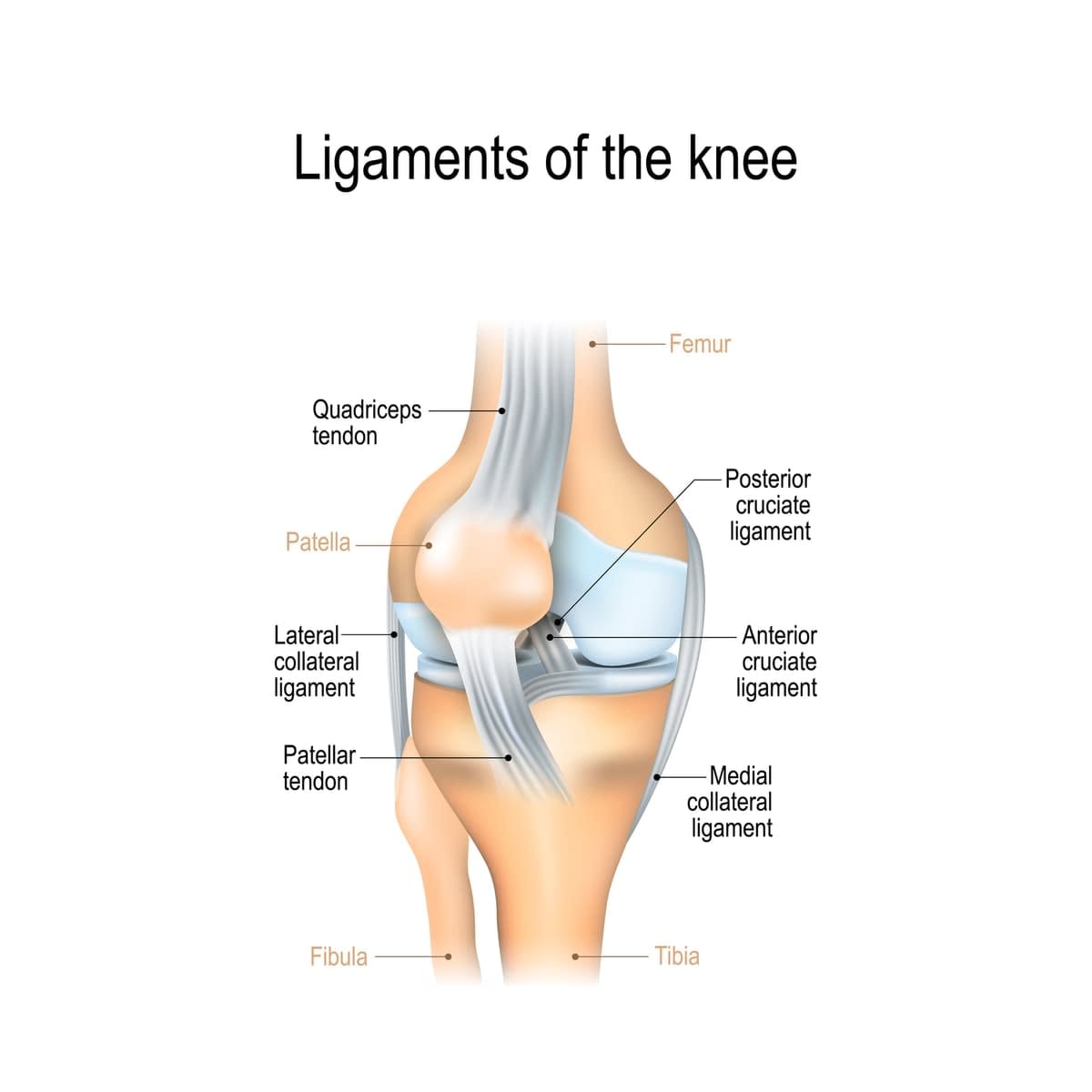
“What we found from the tested cadaver knees,” he said, “was chemical and structural evidence of microdamage of the ACL femoral enthesis”, which is where the ligament attaches to the thigh bone, and where the ACL typically tears.
The results were consistent with ACLs removed from patients undergoing ACL reconstructions.
The anterior cruciate ligament is the primary knee stabiliser, and one of the major ligaments connecting the tibia (shin bone) and femur (thigh bone) bones.
It runs diagonally deep within the knee and is composed mainly of collagen fibres that assemble in a hierarchical order to form the ligament, along with a small proportion of elastic fibres, thereby giving the ACL high tensile strength. Its function is to provide rotational knee stability.
Collagen is often described as the glue that holds our bodies together. It’s the most abundant protein in the human body and, as well as our ligaments, is found in our bones, muscles, skin and tendons.
Turning to ‘jello’
Using atomic-force microscopy to characterise the ACL collagen at a nanometre scale, or one billionth of a metre, Professor Banaszak Holl and his team were able to identify “a consistent unravelling of the molecular structure of the collagen” in the ACLs of the cadaver knees, effectively turning the ligament into “jello”.
“This disruption of the collagen’s helical assembly results in reduced tensile strength and abnormal shape of the collagen fibrils,” he said.
“This damage may, at least in part, be responsible for the reduction in structural integrity that has been shown to lead to non-contact ACL failure during repetitive strenuous athletic manoeuvres.”
Here’s an image of collagen fibrils of a healthy ACL:

“This is a nice smooth ligament, where you can actually see the collagen fibres,” Professor Banaszak said.
And here’s what a repetitive stress injury of an ACL looks like on a molecular scale:

“So, we have all these holes that are about the size of a collagen fibre, where there’s big nanostructure damage,” Professor Banaszak said. “That’s not too surprising, because we know the collagen triple helixes are unwinding, but you can see it as a nanoscale effect.”
Professor Banaszak Holl said the results of this latest research throws into serious doubt the argument that ACL injuries are mostly caused by single-force events and a lack of neuromuscular training.
“The dominant focus here in Australia has been for neuromuscular agility training, and really it has been argued that the problem is not what we’re saying here,” Professor Banaszak Holl said.
“It’s argued that the issue is a single-force event, so we’re making quite a different argument. We’re saying that continued use has generated damage that isn’t repaired at a quick enough rate, to a point where the ligament can’t handle forces that it normally would and should.”
Succumbing younger
Dr Wojtys has been studying the issue for more than 30 years, and in that time has noticed a marked increase in younger and younger athletes and women succumbing to ACL injuries.
“Incredibly, we’re seeing that the peak age for ACL failures is 14 now for females, and in men 17,” he said, attributing the rise to children entering sporting pathways, and increased training loads, at younger ages, and the increased participation of women in sport.
“This will lead to people in their mid-20s suffering from osteoarthritis and other chronic health conditions later in life such as obesity and cardiovascular disease,” he said.
Call for change
The researchers are advocating for changes in training regimes until non-invasive techniques are developed that can determine who might be predisposed to an ACL injury because of submaximal loading cycles.
“It turns out that the kind of problem we know we’re seeing here, we know that the MRI techniques people have been using are tuned up for the wrong thing,” Professor Banaszak said.
“We’re very interested in endoscopes, and it turns out there’s a confocal endoscope made by Optiscan Imaging, which was originally a technology developed and spun out from technology developed here at Monash University, and we’re working closely with them both at Monash University and at University of Michigan to try and translate this research for initial evaluation of the knee problem and for the surgical repair process.
"It’s not worth pushing our bodies and ligaments to the extreme because of the potential long-term damage it can cause. There are limits to what the human body can do."
“The high-resolution imaging and small diameter of their endoscope gives us some unique research and potentially surgical capabilities.
“We’re also thinking now of every non-invasive way we can, and I’m sure other people will, too, once they get our data, to try and come up with ways that let us test for this damage, but non-invasively.”
Until then, Professor Ashton-Miller says, “we have to ask ourselves, is more always better”?
“Until we have more answers, it’s not worth pushing our bodies and ligaments to the extreme because of the potential long-term damage it can cause. There are limits to what the human body can do.
“Less practice, less repetition and less fatigue in our joints and ligaments will ultimately lead to less injuries. And this should be the main focus of sporting clubs and athletes of all ages and levels of professionalism.”





