
“I’ve got some great things to tell you!” says Monash University’s Professor Carol Hodgson, a leading researcher on the effects of intensive care, or ICU. The COVID-19 pandemic has seen a huge surge of patients with the deadly virus into ICUs across the world, on ventilation. Then, for those she calls “ICU survivors”, the rehabilitation begins.
“We know COVID-19 patients on mechanical spend a little longer in ICU than people with other influenzas,” she says. “The duration in ICU is longer, and they may have worse outcomes.”
Professor Hodgson is Deputy Director of the Australian and New Zealand Intensive Care Research Centre at Monash’s Department of Epidemiology and Preventive Medicine. She’s also a senior physiotherapist in ICU at the Alfred Hospital, and former director of trans-Tasman charity the Intensive Care Foundation.
The new research she’s leading will shine a light on the after-effects of a disease such as COVID-19 on a human body after emerging from ICU. It will also highlight the work that physiotherapists do in intensive care.
As this long-read in The Atlantic shows, the “lingering damage” of COVID-19 is largely unknown – befitting its dastardly status as a “novel”, or new, coronavirus. But research on patients is starting to emerge. This Australian study takes patients who have already been enrolled in a short, observational study of severe acute respiratory patients so they can be studied in more depth. It’s essentially a national database of 300 COVID-19 patients from ICUs at 40 hospitals.
“We evaluate their recovery at three and six months, including long-term functional assessments of their physical, cognitive and psychological health. In addition, we’re reporting the physio interventions used in ICU, including early rehabilitation.”
The Covid-Recovery Study will also work towards building a “risk-prediction model for disability-free survival” of the virus.
Guideline for patient management went global
It all began back in March, when the group of senior ICU physios wrote what has become an international guideline for management of COVID-19 patients in ICU. It was published in the Australian Physiotherapy Association’s Journal of Physiotherapy and has since been translated widely, with links to the publication on the World Health Organisation (WHO) website.
“Then, leveraging off that, we thought, ‘Wow’. We were having conversations about COVID-19, and we didn’t know what physio and rehab interventions were effective.”
The team had input from colleagues at the NHS Nightingale field hospital in London, as well as others in Europe. “We didn’t know the long-term outcomes for patients once they had been in ICU, and we thought that would be important research,” Professor Hodgson says.
Read more: Fighting COVID-19 from the intensive care bed
The project is still in its early stages in this country, but data from other countries – in particular, COVID-19 hotspots of Italy and China – is starting to emerge.
“What we can see is that there are very specific issues these patients are left with. Even at three months, up to 40% of them have persistent shortness of breath. These are not new symptoms; this is a population of COVID survivors and patients who had shortness of breath upon presentation to hospital. So, if you were short of breath before, 40% are still short of breath three months later.
“They also have muscle aches, extreme tiredness, and even an ongoing persistent cough for long periods. Similar to other ICU cohorts, at three months they have decreased function and quality of life, particularly around exercise capability.”
What the team wants to establish is whether a COVID-19 survivor from ICU has a different recovery than patients from ICU with other types of respiratory diseases.
“We have data for 1000 ICU survivors from other forms of respiratory failure at three and six months,” Professor Hodgson says. “We’ll be able to do a head-to-head comparison of COVID to non-COVID – this way we’ll be able to tell.”
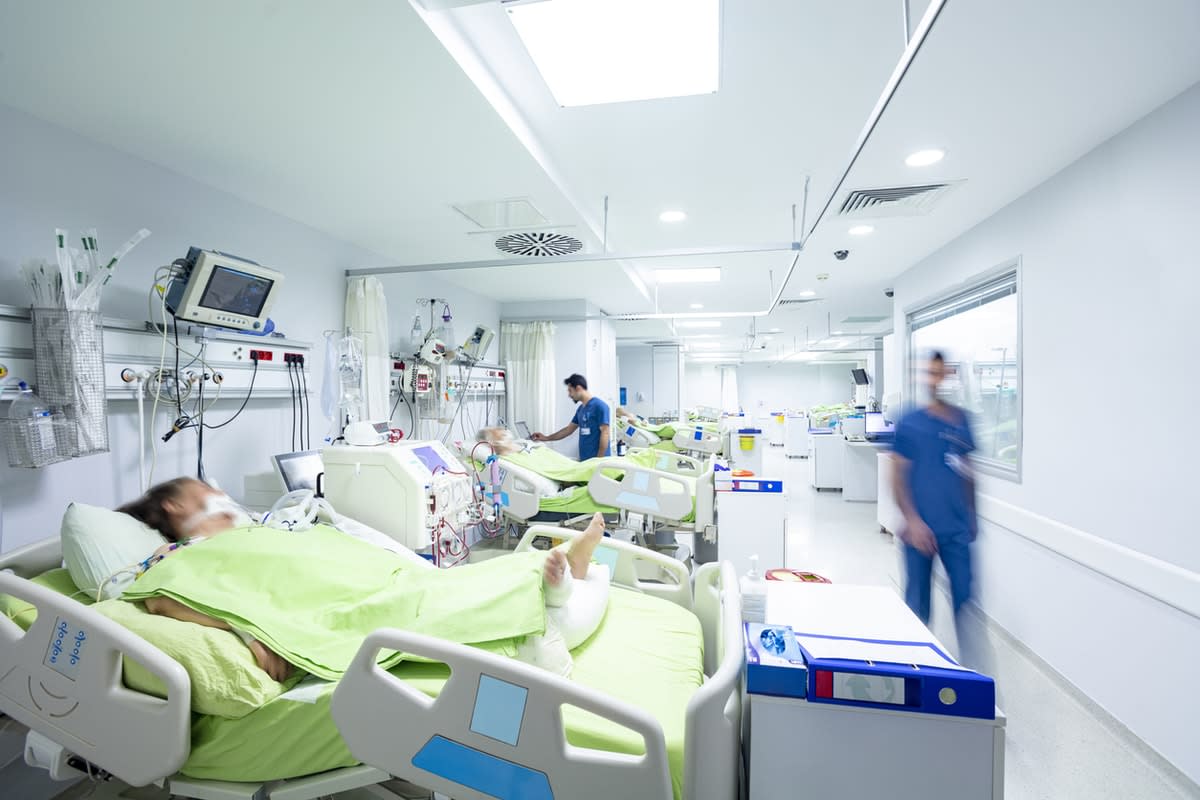
The role of physios in ICUs
Meanwhile, in ICUs in hospitals around the country, physiotherapists are busy dealing with very sick COVID-19 patients.
Here’s how it works.
“We’re experts at assessing respiratory function and starting early rehabilitation,” says Professor Hodgson. “We can optimise ventilation and breathing through positioning for lung expansion and oxygenation. We also know how to manipulate the ventilator to help patients if they have specific areas of consolidation in their lungs.
“More importantly,” she says, “we know now if we just leave our patients lying in bed for seven to 10 days, they can lose up to 20% of their muscle mass. So early rehab is considered best practice in ICU now.
“But COVID patients are harder to rehab because there can only be minimal exposure, everyone is wearing PPE, moving a patient is complex, there’s minimal staff and equipment in the room. The challenges are really, really difficult.”
Dealing with the unexpected
Jason Pereira – who graduated from Monash with a Bachelor of Physiotherapy (Honours) in 2017 – worked in the Alfred Hospital’s ICU for eight months this year, through the two COVID-19 peaks. Professor Hodgson was often there, too. At first, he says, it was “brand-new, no-one knew what to expect. No-one knew what the challenges would be, and how long we would be doing it. Everyone was thrown in the deep end together, but I felt well-supported from the ICU team.
“The first time you walk in you’re nervous and sweating, because you just don’t know what to expect. But the more times you spend with them [the patients] you realise it’s just another patient, only with more layers of protection, and you get down to business.
“There was a fear generated around these patients. We treat quite a lot who are in isolation and very infectious all the time, but because this is a new disease and creates headlines, you aren’t sure how this one was going to be different.”
"Patients are harder to rehab because there can only be minimal exposure, everyone is wearing PPE, moving a patient is complex, there’s minimal staff and equipment in the room. The challenges are really, really difficult.”
A key skill physios bring is turning the patients, or “proning” them – it helps their breathing if they’re on their stomachs. The procedure is carried out by a team of at least seven.
“Physios are very involved, moving the patient from their back onto the side, then onto their tummy. These are very unstable patients. We need to be very careful of oxygenation, heart rates and blood pressure. Everyone is tense. But physios are naturally hands-on, so it’s second nature – we’re used to touching patients and moving them,” says Pereira.
“With COVID patients, we’re very particular about how we position ourselves. If for some reason their breathing tube gets disconnected, everyone is potentially exposed to COVID, so one false move could be potentially harmful. Everyone needs to be on top of their game and really concentrating.”
Read more: Coronavirus: Ventilators are saving lives, but they can also damage lungs
Then there’s the delicate task of rehab, which occurs while the patient is in a coma or awake. “We have to help them maintain strength and range of movement in their arms and legs. We stretch them out while they’re in a coma, or sit them on the edge of the bed while awake and on ventilation. We take a proactive approach to rehabbing these patients. We’re always thinking of the long-term outcomes.”
Professor Hodgson says the results of the Covid-Recovery Study are hard to predict, but it will, at the very least, “increase understanding of the roles that physios are asked to play, and are capable of playing, in a future pandemic or a surge in ICU.”
Even with a vaccine, she says, “we will still see COVID-19 for a long time”. But the study will show better ways of managing patients so they have improved outcomes.
“Physios are extraordinarily resourceful and intelligent people,” she says. “I think we’ll learn that there are a lot of them in ICUs across Australia doing unique and novel things, and that is valuable information to share.”





