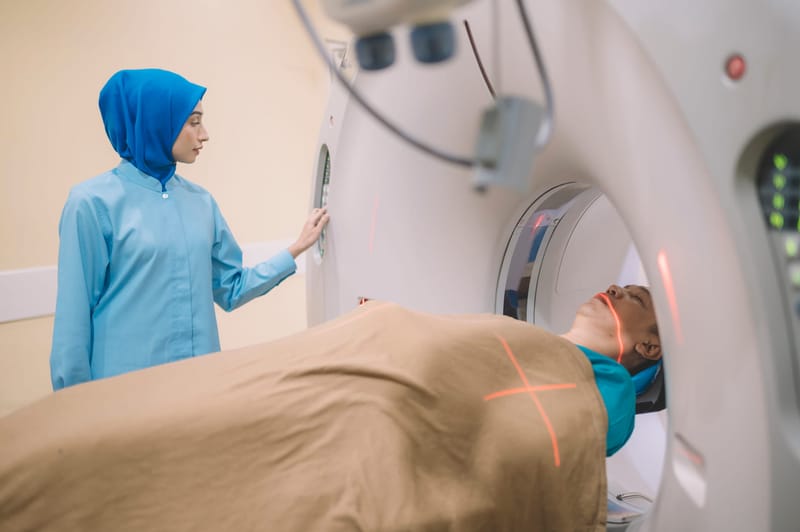
Although recent encouraging news suggests the rate of new coronavirus cases in Australia is slowing, our medical facilities could still be overwhelmed at some point.
One modelling study has suggested that, if public health measures are not observed or do not work, demand for the existing 2200 intensive care unit (ICU) beds in Australia will be exceeded within a few weeks. More optimistic views of our achievable ICU capacity would merely delay this event for a few weeks.
Critical shortages of ICU beds and other medical resources overseas have resulted in large numbers of deaths. In these countries there have been vigorous debates about which of many eligible patients should be given access to care facilities in short supply.
This discussion is now underway in Australia.
For many clinicians, the question of who has access to limited ICU beds presents disturbing challenges, especially in view of a widely disseminated proposal that has gained particular support in Italy. This bases decisions about who is granted access to ICU beds on calculations of the future years of life that could potentially be achieved through treatment (or, in some proposals, “quality-adjusted” years of life).
This would deny access to people above a certain age, as well as to people with disabilities and certain medical conditions.
Read more: People with a disability are more likely to die from coronavirus – but we can reduce this risk
What is a person worth?
This approach is deeply problematic.
It has taken many years for us to move away from judging the value or worth of a person by their age, race, sexual preference, physical ability, religion or other personal characteristics.
The worst outrages of the 20th century resulted directly from such approaches, which were often claimed at the time to be supported by “ethical” justifications.
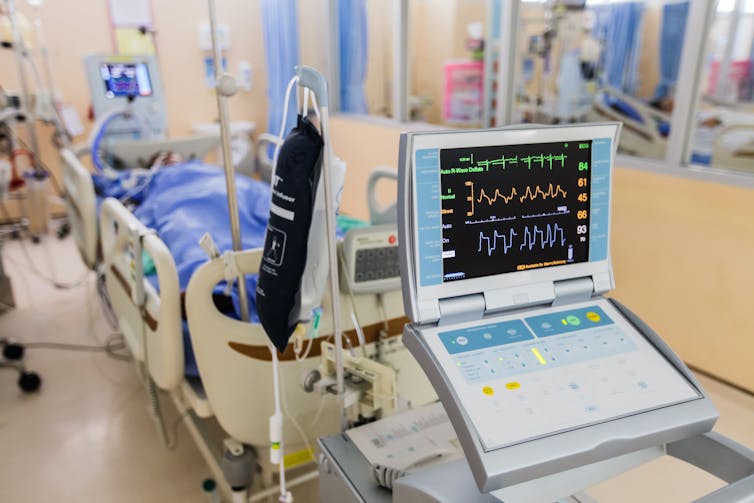
There's also never been a public discussion, and certainly there is no agreement, about whether the “ethical value” of a person can be calculated mathematically on the basis of the total number of years he or she might live.
The alternative, which has been developed and routinely employed in hospitals around Australia for years, applies a process of rigorous discussion about the potential benefits and burdens of treatments proposed for every individual patient, taking into account all relevant clinical features and whether acute problems can be overcome.
It entails a detailed analysis of technical issues and results. It involves open discussion with the patient, medical carers, family members and expert ICU staff, about medical, social, emotional and ethical issues.
It embraces flexibility and a readiness to adapt and change protocols with changing circumstances. It takes into account the specific circumstances of individual patients’ lives, including their personal preferences and religious and cultural beliefs.
It leaves aside personal characteristics not relevant to the medical decision at hand, such as race, gender, sexual preference and ethnicity.
Age can be relevant
This is not to say that age can never be a relevant consideration. Indeed, in some conditions, advanced age is closely linked with the likelihood of a poorer response to a treatment.
Sometimes this is because increasing age is directly linked to age-related diseases that reduce the likelihood of a successful outcome from treatment, such as certain types of cancer.

At other times, for reasons that are much less clear, age itself appears to predict poor outcomes of treatment, leading to its inclusion in many scoring systems for predicting outcomes of treatment, including in intensive care and cancer care.
In both cases, it's valid that age be taken into account in decision-making. It's also possible that age may be relevant to more philosophical considerations – for example, whether older people consider themselves to have already lived a “fair innings”, or whether young people should be given the opportunity to live a life and gain their potential.
Read more: The 'dreaded duo': Australia will likely hit a peak in coronavirus cases around flu season
While these may also be relevant considerations, and be accepted by many, including sometimes by older people themselves, they are much less clear and much more contested, and require ongoing debate.
The key point is that, even in these cases, age is never taken as a defining quality or characteristic of a person, but rather as a potential signifier of other relevant characteristics or risk factors. Its relevance is linked to what it implies for the particular person, not to an assumption that old people have diminished value and are less worthy of treatment.
In extreme settings, time and resource constraints may add greatly to pressures on the decision-making process, but the same principles still apply. In fact, it's exactly in these contexts that it's most important to resist resorting to criteria that are not founded on evidence or valid ethical arguments.
How do we respond?
The ethical strength of a society is revealed in how it responds to serious challenges. If we have values worth defending, this is the time to fight for them.
Most of us don't want to move to a society based on the arbitrary imposition of measures that discriminate against people on the basis of ethically or medically irrelevant personal characteristics.
Future generations will judge us on how we respond to this crisis, and whether we've been able to defend our core values. This is the time, perhaps more than any other, when we have to keep our ethical nerve.
Read more: How we'll avoid Australia's hospitals being crippled by coronavirus

This story was co-authored by George Skowronski, Research Affiliate, Sydney Health Ethics, School of Public Health, University of Sydney; and Ian Kerridge, Professor of Bioethics and Medicine, Sydney Health Ethics, Haematologist/BMT Physician, Royal North Shore Hospital, and Director, Praxis Australia, University of Sydney. The authors do not work for, consult, own shares in or receive funding from any company or organisation that would benefit from this article, and have disclosed no relevant affiliations beyond their academic appointment.
This story originally appeared on The Conversation