
Annie Makar, a respiratory scientist working on Monash University’s landmark Hazelwood Health Study, is in a small room at a health clinic in Morwell putting a peg on a lady’s nose.
Before them is an array of lung function measuring equipment. The lady’s name is Dianne Godden, 57 (pictured); she lived through the Hazelwood coal mine fire in Gippsland in 2014, which, we are beginning to learn, may have serious health consequences for some of those who inhaled its toxic smoke for up to 45 days.
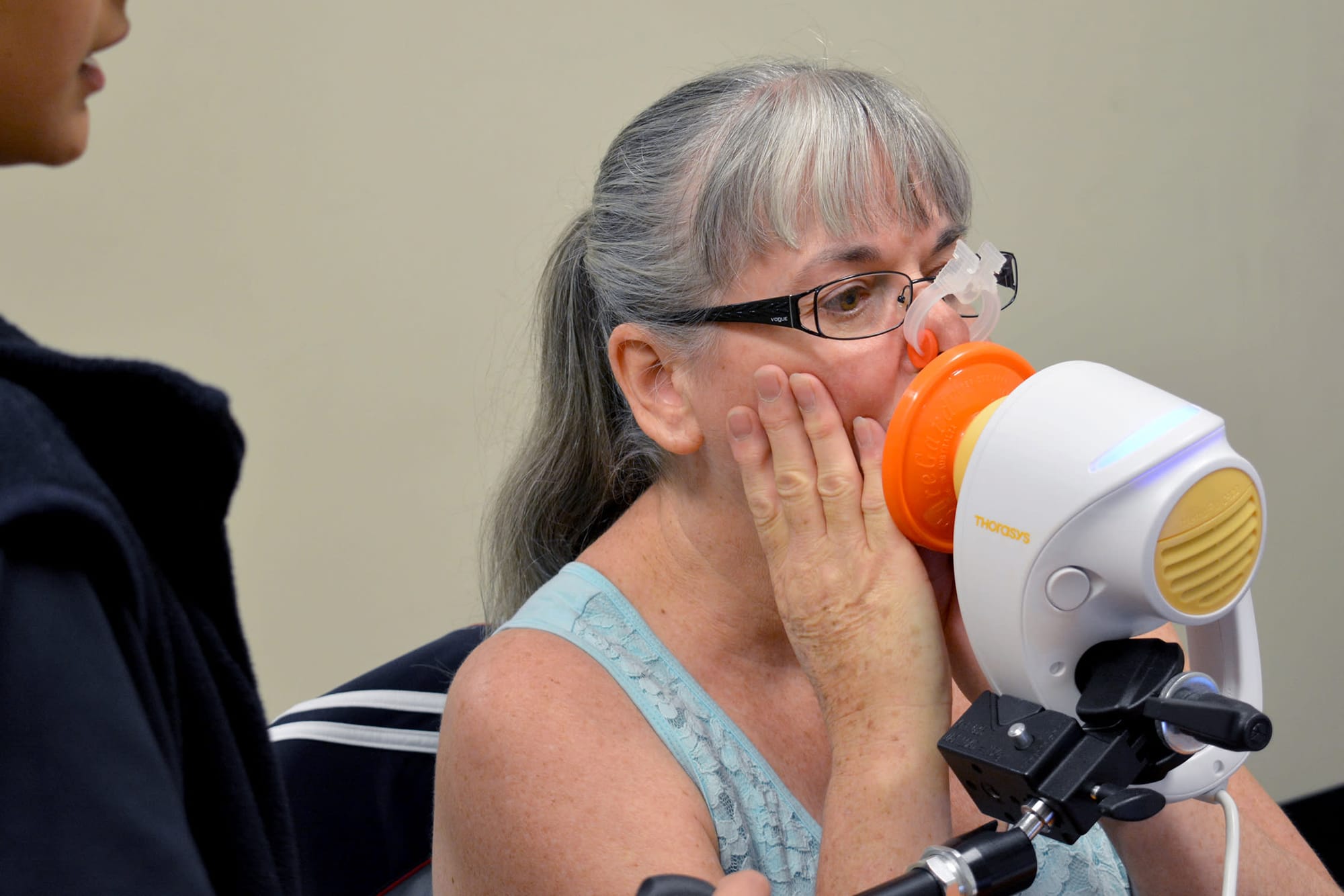
The Hazelwood Health Study is led by professors Michael Abramson and Judi Walker from Monash University’s School of Public Health and Preventive Medicine (SPHPM) and the School of Rural Health. It's the largest environmental health survey of its kind in the world, run by a team of world-leading disease detectives. It has three other universities as partners, plus the CSIRO.
Annie, who is part of the Hazelwood Health Study Respiratory Stream coordinated by Brigitte Borg, usually works at the Alfred Hospital’s Respiratory Physiology Service. But they've relocated to Morwell or Sale for the duration of the Respiratory Stream’s five-month data collection, while Brigitte visits once a week.
The Victorian Government Department of Health and Human Services-funded Hazelwood Health Study is exhaustive. It will probe heart and lung health, the health of those who were pregnant, the health of old and young people, as well as mental health, cancer and broader community wellbeing. Lung studies began in August with about 300 people who had already contributed to a more general adult health survey. The same volunteers – who may or may not be sick from the smoke – will be tested again in three years and then again in six years.
The Monash SPHPM has already investigated a breast cancer cluster at ABC studios in Queensland, and also a spike in black lung diseases in Queensland. SPHPM is advising on the health effects of the Grenfell disaster in London, and recently published a national study of paid and volunteer firefighters – the first of its kind in world – showing an increased risk of prostate cancer associated with the number of fires attended. In effect, the Monash research will be a real-time study that may have implications not only for communities exposed to coal mine fires, but also for those exposed to high levels of industrial air pollution in, for example, China or India.
Two government inquiries have found smoke from the Hazelwood fire was the likely cause of some Latrobe Valley deaths. The owners of the brown coal mine, led by French parent company Engie, face court this year to answer charges of causing air pollution and a “noxious or poisonous or offensive” atmosphere.

And so, at community level, Dianne’s nose is pegged by respiratory scientist Annie as she prepares to begin her two-hour, one-off suite of lung function tests. “This one is called the FOT – the Forced Oscillation Technique,” says Annie. It's one of five tests carried out on an individual – the team tests six participants a day. In FOT, sound waves are reflected from the lungs during breathing exercises to measure resistance – healthy lungs have lower resistance. The results play live on a screen before her.
“Now we'll start the vibrations,” says Annie. Dianne is breathing into the FOT machine, which looks not unlike a pig’s snout. “Keep breathing, take a deep breath in, not too fast, not too slow. Now blow all the way out. A little slower, keep going, pushing it that last little bit more – and back to normal breathing. You’re doing a wonderful job.”
Dianne was working for the local council when the coal mine caught fire in the summer of 2014. Thousands of residents of Morwell and nearby towns were smoke-affected – it was billowing through their homes on the whim of the wind for nearly six weeks. Some were voluntarily relocated. The problem was the PM2.5 particles – very small airborne matter of or less than 2.5 thousandths of a millimetre in diameter. These can go deep into the lungs or enter the bloodstream. All she could do was stay inside and keep the house shut, then open it when the wind changed, then shut it again. Her employer shifted most council work indoors.
For Dianne, being one of 340 participants in the Respiratory Stream – a ‘participant’, not a ‘patient’, because they might not be sick – is about the public good. “I think it’s important that people who don’t have political agendas participate, just normal citizens. And of course I'm interested to find out if I have been affected.”
The tests for her and everyone else who put their hand up include two novel techniques in the FOT and also the multiple-breath nitrogen washout, which evaluates how evenly gases move in the lungs. The more routine tests of spirometry (measuring the volume of breath being forcibly exhaled) and measurement of gas transfer are also used.
According to Monash’s Professor Bruce Thompson, the Respiratory Stream lead and head of the Physiology Service at the Alfred Hospital’s Respiratory Medicine unit, the best result for the community would show the disastrous coal fire had no effect on population health. But he doubts that it will. He cites a study in New York after the September 11 Twin Towers’ collapse that showed high concentrations of highly alkaline crushed concrete, gypsum and synthetic vitreous fibres (SVFs) were inhaled.
“We're trying to find whether the event at Hazelwood has any effect on lungs,” he says. “In six to 10 years it should become really evident. If we start to see major changes within that time, we know we have a big problem.”
Initially, says Tracie Lund, who chairs the study’s community advisory committee, locals were not overwhelming in their willingness to be tested because they misunderstood what it was for and still felt angry about a perceived slow state government reaction to their plight during the event. But she says now the Monash-led teams in Morwell are treated like “community champions” because people understand the study has their interests at heart (and lung).
For respiratory team coordinator Brigitte Borg, investigating the health of participants rather than patients is a “completely different scenario” than clinical work in a hospital. “We're looking for outcomes of the direct result of an event,” she says. Data collection for this stream will end around February 2018, with preliminary results to follow at the end of the year.





