With COVID-19 affecting our daily lives, many Australians are asking: What happens if I test positive? With no known cure and no vaccine, what are my treatment options?
Finding trusted answers amid the widespread coverage of questionable claims and dubious data on unproven treatments isn't easy. The good news is there are clear guidelines and growing evidence on treatments that can have a dramatic effect on COVID-19.
Here’s a snapshot of how this knowledge and guidance is likely to apply to you, if you have mild, moderate or severe COVID-19.
Read more: How are the most serious COVID-19 cases treated, and does the coronavirus cause lasting damage?
Testing positive and isolating at home
If you test positive, you must self-isolate at home. Your local public health service will contact you with advice and information about how long you’ll need to do so.
If you're like most people with COVID-19, you won’t need to go to a clinic or hospital, and can safely self-manage the illness at home. Even so, it’s important to connect with an appropriate healthcare service (either by contacting a dedicated COVID-19 service or by calling your GP) for an initial assessment and continuing contact throughout your illness.
Initially, you may experience flu-like symptoms such as cough, sore throat, fever, aches, pains and headache. You might temporarily lose your sense of smell and taste; less common symptoms include nausea, vomiting and diarrhoea. Whatever your symptoms, you’ll need plenty of rest, fluids and paracetamol for aches, pains or fever.
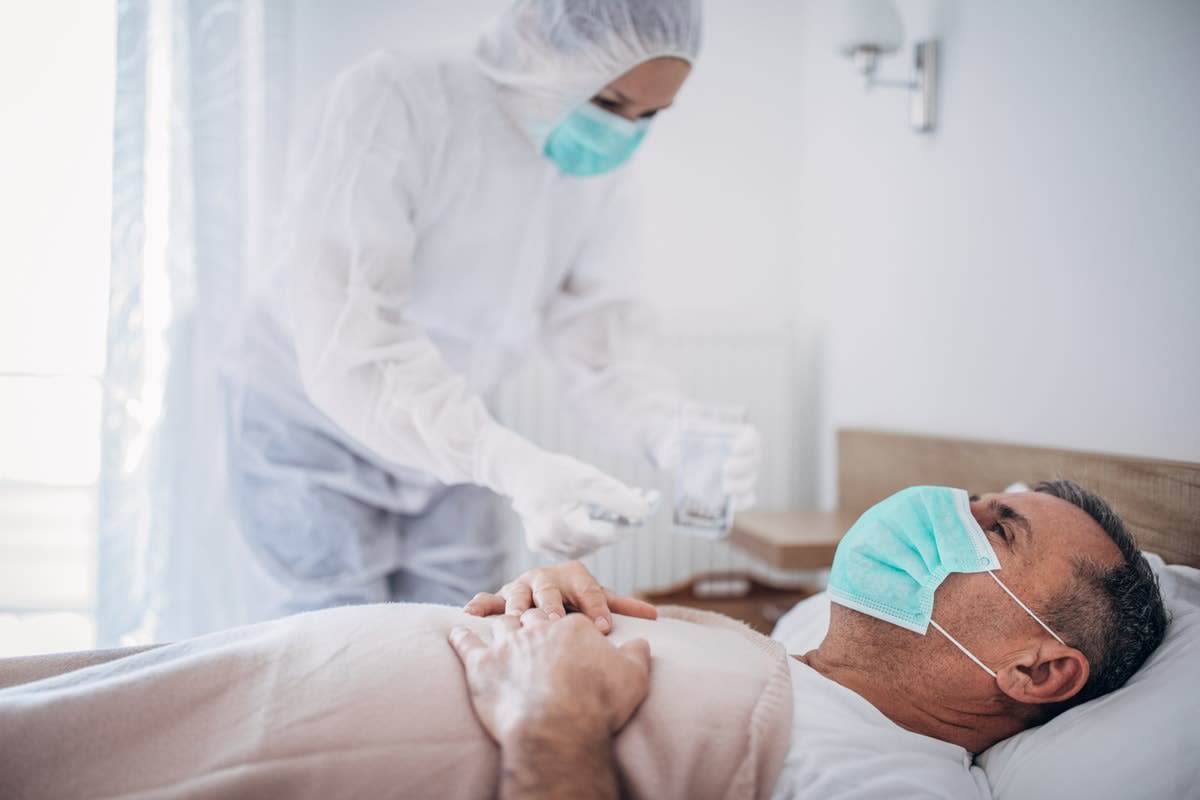
Take particular note of how you’re feeling from day five onwards, as this is the time some people begin to deteriorate significantly. About 20% of people fall into this category, with older people and those with pre-existing health conditions more likely to require hospitalisation. Watch out for intense fatigue, difficulty breathing, or an overall deterioration in how you’re feeling.
If your symptoms worsen, you’ll need to contact your care provider, or if your symptoms are very serious (such as difficulty breathing), call 000 and ask for an ambulance, and don’t forget to tell them you have COVID-19.
What if things get worse still?
If you're taken to hospital, doctors will measure your oxygen levels and perform a chest X-ray and blood tests to determine whether you have pneumonia (infection in the lungs, which is a sign of moderate or severe COVID-19). If pneumonia, low oxygen levels or other signs of severe infection are detected, you’ll need to stay in hospital and will probably be given oxygen.
If this is the case, you’ll also be given a strong anti-inflammatory medicine called dexamethasone. This is a widely used, low-cost drug that was recently found to reduce the risk of dying from COVID-19 (by 15% for people on oxygen, and by about a third for people on a ventilator). However, for people who are not on oxygen, dexamethasone may increase the risk of death — probably because inflammation is not such a big factor at that stage of disease — and the side-effects of dexamethasone would outweigh any potential benefit to those patients.
Read more: Dexamethasone: the cheap, old and boring drug that's a potential coronavirus treatment
For moderate or severe cases, doctors may also consider a newer antiviral medicine called remdesivir. Originally developed to treat Ebola, this drug has recently been shown to reduce the time to recover from more severe forms of COVID-19 — but not to reduce the risk of dying from the disease.
Read more: Remdesivir explained – what makes this drug work against viruses?
If you become even more unwell, these treatments will continue, but you may need more support for breathing, such as high-flow oxygen or a ventilator, and will likely be cared for in an intensive care unit.
The recovery journey
Your recovery depends on many factors, including your previous health and fitness, and how sick you became with COVID-19. The recovery phase is not yet fully understood, but we do know some people suffer prolonged symptoms, including fatigue, breathlessness, and joint and chest pains.
Read more: Here's what we know so far about the long-term symptoms of COVID-19
As scientists continue to grapple with the complexities of understanding and treating this virus, we'll have more questions than answers for some time yet.
Fortunately, Australia moved quickly at the start of the crisis to establish a National COVID-19 Clinical Evidence Taskforce. A collaboration of 29 peak national health organisations, the taskforce works around the clock to rapidly identify, evaluate and summarise global COVID-19 research findings. Each week, guideline panels with more than 200 experts use this evidence to review and update national “living guidelines” to inform consistent, high-quality patient care around the country.
This pace of updating rigorous, trustworthy guidelines weekly is a world first. Whatever the global headlines or social media outrage of the day, Australian health workers will continue to have a single, accessible source of consistent, evidence-based guidance in a time of great uncertainty.

This story originally appeared on The Conversation