When the Victorian Administrative and Civil Tribunal (VCAT) last year rejected a new liquor store application in the regional town of Daylesford, the decision drew on key evidence from publicly-accessible health data.
In its findings, the tribunal considered statistics provided to the community by Turning Point via AODstats, which identified higher hospital admissions for alcohol-related harms in the local government area in 2022, alongside elevated rates of alcohol-related serious road injuries and deaths.
Professor Dan Lubman AM, Executive Clinical Director of Turning Point and Professor of Addiction Studies at Monash University, says the case highlights a broader shift in how research reaches the public.
“Historically, much of the evidence about alcohol and other drug harms sat with researchers or policymakers,” he says. “With the AODstats platform, we’re now seeing research data being translated into open resources that communities themselves can use to understand what’s happening where they live.”
A new lens on emergency health data
The AODstats platform, developed by Turning Point in partnership with Monash University and the Victorian Department of Health and launched in 2014, provides the state’s most up-to-date publicly-available information on harms related to alcohol, illicit and pharmaceutical drug use.
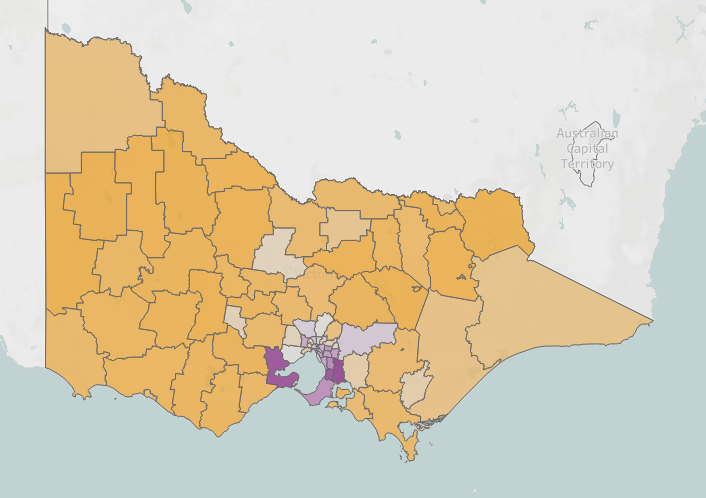
Drawing on data from more than a dozen sources across the past decade, the platform allows users to explore alcohol and other drug harms through interactive maps, demographic profiles and trends over time.
This long-term view is one of its greatest strengths, researchers say, enabling users to examine how patterns of harm shift whether in response to major social events, natural disasters or changes in policy.
A key feature of AODstats is its integration with the Victorian arm of the National Ambulance Surveillance System (NASS), an internationally-unique dataset derived from the structured coding of paramedic clinical data, capturing acute ambulance attendances involving alcohol, illicit and pharmaceutical drugs, mental health crises and self-harm.
Researchers explain that ambulance data occupies a distinctive space in the health system, documenting incidents at the point of crisis, often before people present to hospitals or enter formal treatment pathways, and providing insight into harms that might otherwise go unrecorded.
“From a scientific perspective, we know that the system is robust and allows us to see patterns that traditional data sources miss,” explains Dr Rowan Ogeil, Strategic Lead of Turning Point’s National Addiction and Mental Health Surveillance Unit (NAMHSU).
“It reveals the immediate burden on emergency services and offers an early signal of emerging risks,” he says. “Importantly, it also provides a democratised model that can be adapted in other countries or health systems where ambulances play a critical role in alcohol and other drug care.”
Over the past decade, Monash University researchers have refined the analytical methods underpinning this data, demonstrating how ambulance information can be transformed into a rigorous and replicable public health surveillance system.
What the data revealed during the pandemic
During the COVID-19 pandemic, Monash researchers worked with the AODstats team to track changes in alcohol-related harms as restrictions reshaped daily life. The data pointed to a shift away from licensed venues and into private settings, reflecting broader pressures associated with stress, isolation and economic uncertainty.
Turning Point research fellow Jessica Killian, who has managed AODstats since its launch, says these insights underscore the value of longitudinal datasets. Further research using an extended NASS dataset revealed substantial increases in complex presentations.
“Alcohol-related ambulance attendances involving mental ill-health increased substantially during this period,” she says, pointing to rises of 40% in metropolitan Melbourne and 25% in regional Victoria.
“Ambulance attendances involving both alcohol and suicidal behaviours also increased, suggesting that extra supports and services are needed for individuals with co-morbid alcohol harms to ensure that their clinical needs are being met.”
Seeing risks that might otherwise remain invisible
Beyond pandemic research, Monash-led analyses have used ambulance data to explore patterns of violence, injury and vulnerability.
Researchers have examined alcohol’s role in intimate partner violence, as well as presentations involving children in out-of-home care and other at-risk groups.
The data has also been used to better-understand risks faced by emergency service personnel. By mapping patterns of aggression and violence towards paramedics, including when and where incidents occur, researchers aim to inform prevention strategies and workforce training.
In some cases, ambulance surveillance has highlighted emerging trends before they become widely recognised. Analyses have identified increases in GHB-related harms, regional service pressures and seasonal spikes in alcohol-related incidents, informing planning by health services and policymakers.
Dr Ogeil says the greatest value in the data lies in its ability to identify people at risk who might otherwise go undetected – “those at risk of being injured as a result of alcohol-related violence”, he says.
“We also created pre-implementation comparison data before the introduction of SafeScript, providing vital evidence for researchers evaluating prescription monitoring policies and informing clinical and public health responses.”
Open data and the future of policy
For Professor Lubman, the significance of platforms such as AODstats lies not only in the research they enable, but also in how they reshape the relationship between data and the public.
“When high-quality evidence is openly available, it changes who can participate in conversations about health and safety,” he says. “Communities, local governments and service planners can draw on the same information as researchers, supporting more transparent and informed decision-making.”
The Daylesford tribunal decision illustrates how open access to health surveillance can extend the reach of academic research into everyday policy contexts.
Monash researchers are continuing to expand ambulance surveillance nationally. They hope the approach will strengthen prevention strategies and improve understanding of alcohol and other drug harms across Australia.
“A decade into this work, open science is helping move knowledge from research into real-world decision-making,” Professor Lubman says. “It’s not just about publishing papers – it’s about creating practical tools that support earlier, evidence-informed responses to risk.”