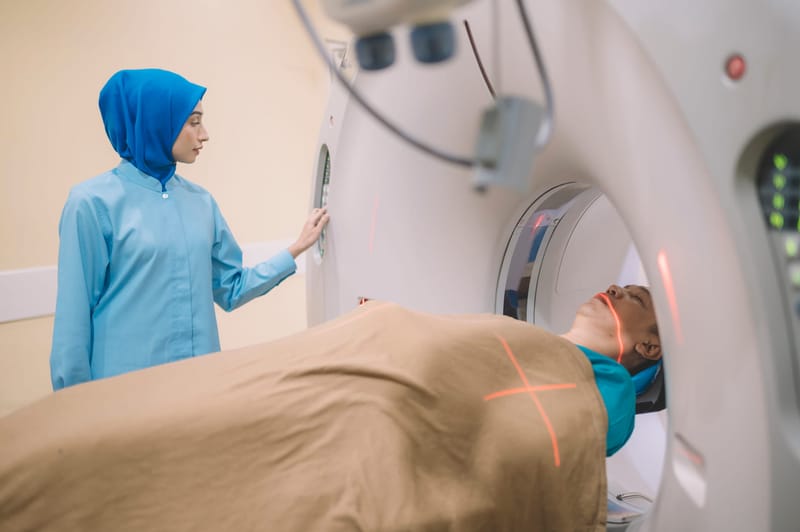
Tim Tran is a clinical pharmacist working on hospital surgical wards at Austin Health in Melbourne. This means he gets to see up-close the effects of invasive surgeries such as knee and hip replacements on his patients. He also has a detailed understanding of the systems in place for providing strong opioid pain medications for these patients when they go home.
Amid a global opioid crisis, Tran’s ongoing research as a Monash University PhD candidate into use of pain medications – particularly oxycodone – is timely. Two published papers he’s co-led this year reveal:
- More than half of the patients were still using opioids three weeks after being discharged from hospital following knee or hip surgery. These patients required ongoing pain management from their general practitioner (GP).
- Discharge summaries provided to GPs for patients leaving hospital after surgery often provided little or no guidance regarding the post-discharge opioid plan. Only 12.8% of summaries in a survey of 285 patients contained an opioid management plan.
A need for a more nuanced approach
Tran is finishing his PhD through the Centre of Medicine Use and Safety at the Monash Institute of Pharmaceutical Sciences. Internationally, several measures have been promoted to simply reduce the quantity of opioids provided to post-surgery patients once they go home, but Tran’s research has shown a need for a more nuanced approach, centred on the patient’s needs.
Those who are “opioid-naive”, vulnerable, or not monitored and supported correctly, may then run into trouble with the highly addictive pain relief.
“I deal with a lot of patients who have had complex and very painful surgeries. You see the impact that restrictions on opioid medications can have on these patients, so I wanted to look at the issue from a patient perspective. What can we be doing to support patients through this time, rather than simply cutting down supplies for all patients?”
The usual scenario now, when a patient is discharged after about four or five days in hospital, is for the surgical team to estimate how much pain relief the patient will need at home, based upon usage in hospital. Once the patient leaves the hospital, their community GP takes on the responsibility for providing ongoing pain relief. Usually, a patient will be given a week’s worth of pain relief by the hospital – or two weeks at the most.
Those who are “opioid-naive”, vulnerable, or not monitored and supported correctly, may then run into trouble with the highly addictive pain relief. Some may require ongoing opioid prescriptions beyond three months after their surgery.
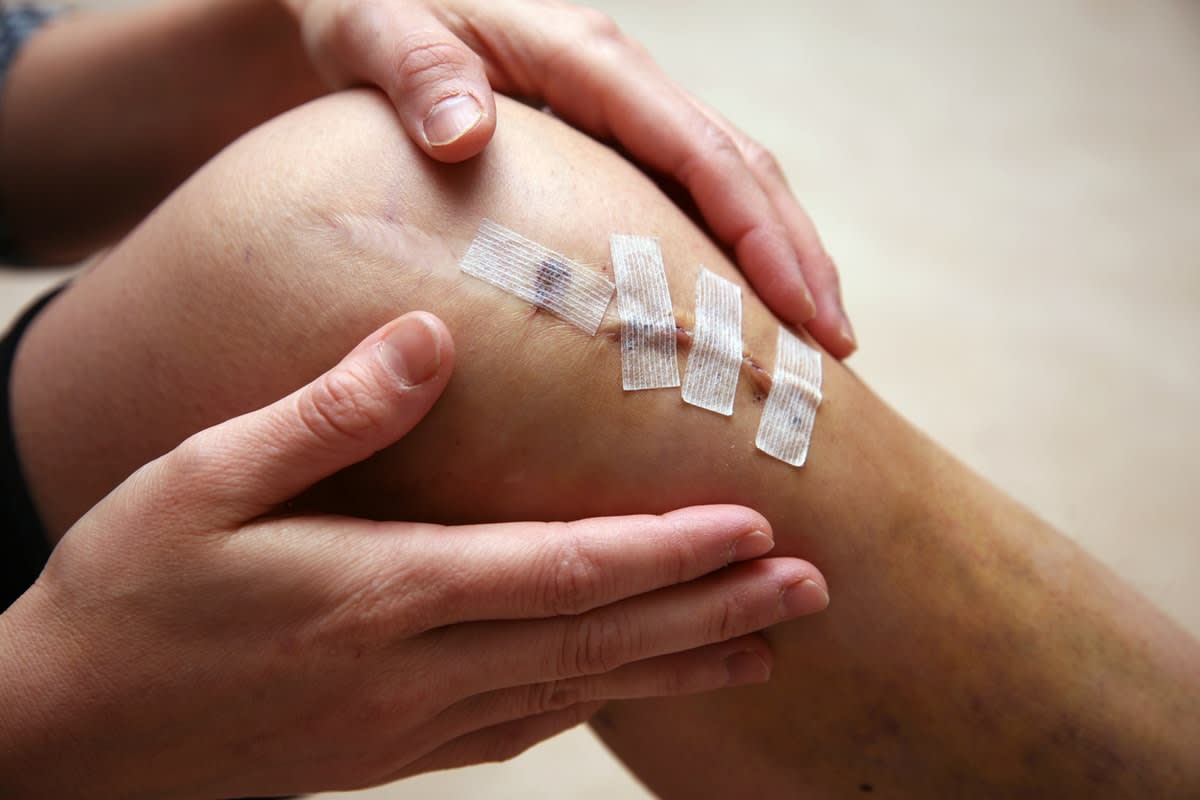
One of the studies that Tran co-led, published in the Journal of the North American Academy of Orthopaedic Surgeons, found that 75% of patients following major orthopaedic surgery had used the majority of their opioid medications supplied from hospital, and that more than half of the patients required ongoing supply. About 5% of these patients developed prolonged opioid use (more than three months’ use).
That paper, published in March, had fellow Monash Institute of Pharmaceutical Sciences researchers Dr Johnson George and adjunct Associate Professor Rohan Elliott as co-authors.
It concluded, in part: “… future research should focus on identifying patients at risk of prolonged opioid use, and improving the transition of these patients into the community”.
“There needs to be a balance between ensuring that we’re addressing the patient’s concerns about their pain and rehabilitation, but also not contributing to the problem within society."
Tran says there’s much room for improvement in the way these patients transition from hospital into the community, and in the quality and accuracy of information provided to GPs to help their ongoing pain management.
“When we discharge patients from the hospital, we’ve always tried to predict the quantity of pain medications they would need when they go home,” he says.
“We didn’t know what happened to these patients after they left the hospital, but we started to receive feedback from patients and physiotherapists that some patients may not have not been supplied with enough pain medication to control their pain and enable them to complete their rehab. On the flip side, we were well aware of the problems that oversupplying opioids can have on the community.
“There needs to be a balance between ensuring that we’re addressing the patient’s concerns about their pain and rehabilitation, but also not contributing to the problem within society – which is that there are excessive quantities of prescribed opioids floating around.”
Discharge summaries must be accurate
This is where accurate and comprehensive discharge summaries are essential, according to Tran. His paper, published in the Australian and New Zealand Journal of Surgery this year, not only found that discharge summaries were often left wanting – in terms of addressing opioid use and supply as patients transition from hospital to the community – but also that a majority of GPs surveyed “rarely or never” received an opioid management plan (within or separate from a discharge summary) at all.
Read more: Can new opioid restrictions stop leftover medicines causing harm?
“From a hospital perspective,” he says, “in many cases, we’re probably oversupplying opioids for simple surgical procedures, but there are some procedures where patients clearly need these medications for a period of time. These are the patients who need us to consider how we can better support them, so that they don’t go on to become prolonged or chronic opioid users.
“What we’ve seen is that GPs are not provided with accurate information or an ongoing management plan for opioid medications initiated in hospital, and in some cases GPs may require assistance in managing more complex patients. This is an important area I see we need to work on further. I think we need to individualise patients’ pain management, rather than just having a simplistic strategy of cutting down the quantities of strong pain relief prescribed for everyone.”
Tran’s current project looks at how hospital pharmacists can contribute to improving communication between the hospital and community health professionals, and supporting patients after discharge. Currently, some hospitals run a pharmacy outreach service to review and support patients who are at risk of medication-related problems once they go home.
He says such services could be extended to include patients who may be at risk of prolonged opioid use.
“Hospital pharmacists can assist in the transition of these patients into the community by ensuring that GPs have accurate information on the pain medications that have been supplied for use after leaving hospital.
“Mechanisms need to be in place so that GPs can also refer their patient back into the hospital system for timely review by pain specialists, if pain is more difficult to manage than initially anticipated. This will ensure that these high-risk medications are reviewed, and not continued for an excessive period of time.”